Edge to Edge Coverage
Uniquely designed soft, flexible, “S” shape provides Edge-to-Edge coverage
CIRCA esophageal temperature probes are designed to deploy 12 sensors throughout the esophagus, positioning the sensors throughout the length and width of the esophagus, ensuring sensor proximity close to the point of treatment. Once properly positioned, the probe’s position is stationary and does not require further manipulation to relocate the temperature sensors.
Importance of temperature sensor location
In addition to the responsiveness of the temperature sensor, position of the sensor is vital to accurate measurement of esophageal temperature.
Studies have demonstrated that a temperature sensor which is just 2mm from the source of a temperature rise will result in a measurement which is lower than the peak temperature.1
The same study demonstrates that the further the sensor is from the source of a temperature rise, the greater the disparity between the measured temperature and the peak temperature in the esophagus. An improperly positioned temperature sensor may provide inaccurate information for the clinician.
Linear probes are prone to lateral (side-to-side) positioning. Studies show that 57% of the time, a straight probe will be located either to the far right or right side of the esophagus, rather than in the middle of the esophageal lumen.5
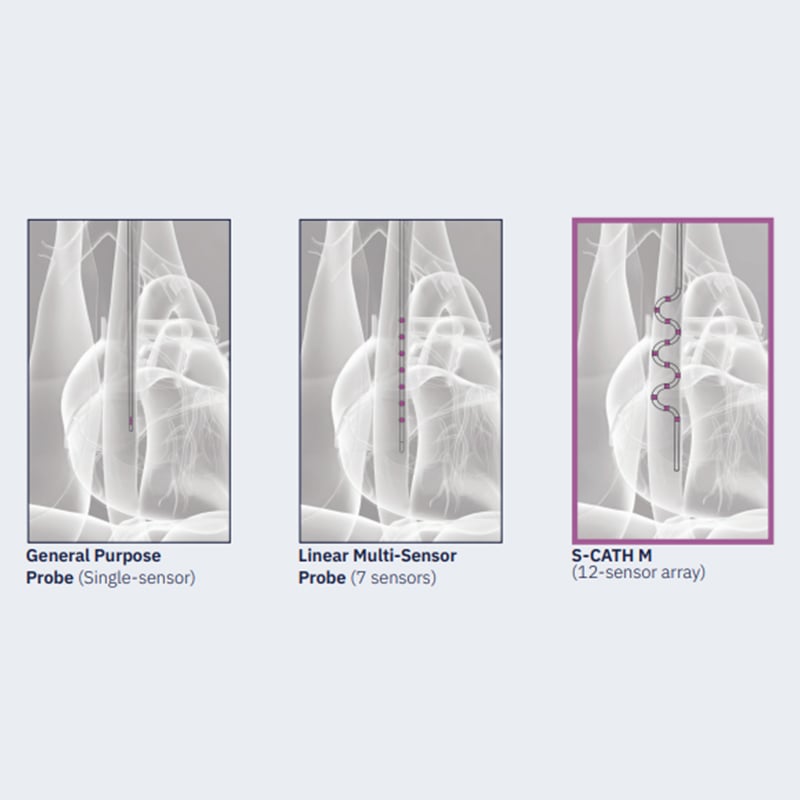
In an independent prospective study of 198 applications in 10 patients, a temperature rise of >2.0°C was recorded 40 times by the S-CATH. Single sensor probes missed 90% of those temperature rises.
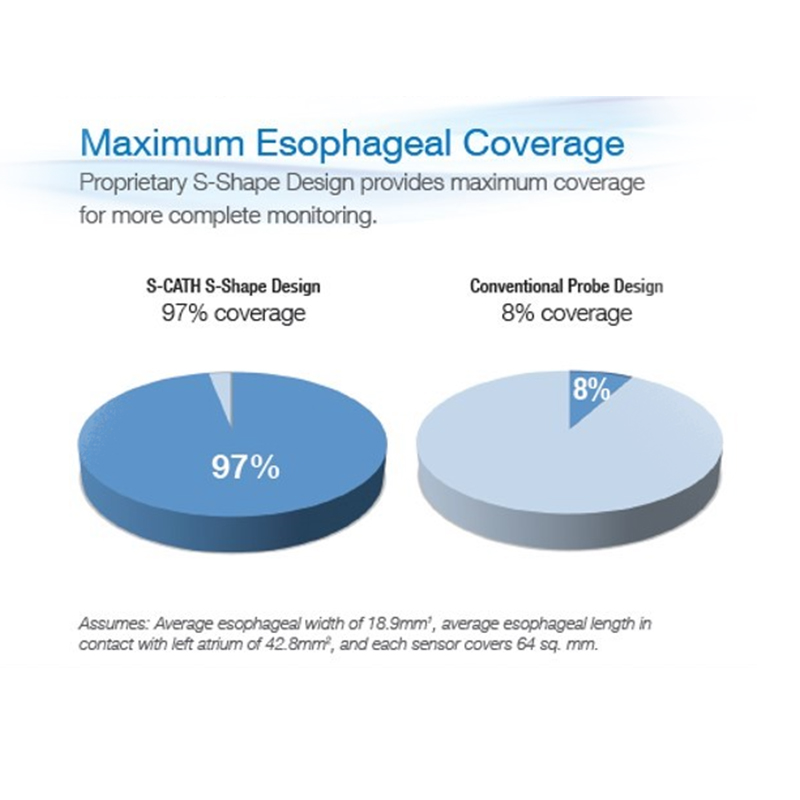
Once properly positioned, the S-Cath’s 12 temperature sensors provide maximum Esophageal Coverage. On average, the S-Cath’s S-shape temperature sensors cover 97% of the esophagus. Using the same methodology, a single sensor covers just 8% of the esophagus in any single position.
Resources
S-CATH M Promotional Video
S-CATH Brochure
CIRCA Temperature Monitoring Overview Video
Ready to learn more about the importance of temperature sensor location?
Click the button below to trial CIRCA’s esophageal temperature monitoring solutions.
References
1. Cury RC, Abbara S, Schmidt S, Malchano ZJ, Neuzil P, Weichet J, Ferencik M, et al. Relationship of the esophagus and aorta to the left atrium and pulmonary veins: Implications for catheter ablation of atrial fibrillation. Heart Rhythm 2005; 2:1317-1323.
2. Tschabrunn, CM, et al., Comparison between single- and multi-sensor oesophageal temperature probes during atrial fibrillation ablation: thermodynamic characteristics, Europace 2015 doi:10.1093/europace/ euu356.
3. Sánchez-Quintana D, Cabrera JA, Climent V, Farré J, de Mendonça MC, Ho SY. Anatomic relations between the esophagus and left atrium and relevance for ablation of atrial fibrillation. Circulation. 2005;112: 1400-1405.3.
4 In-house data. Test conducted by CIRCA Scientific.
5 Knecht, S., et al. “Reliability of Luminal Oesophageal Temperature Monitoring During Radiofrequency Ablation of Atrial Fibrillation: Insights From Probe Visualization and Oesophageal Reconstruction Using Magnetic Resonance Imaging.” EP Europace 19.7 (2017): 1123-1131.